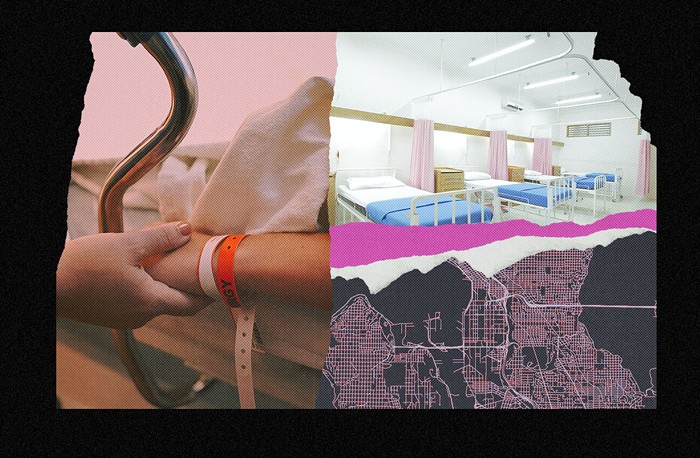
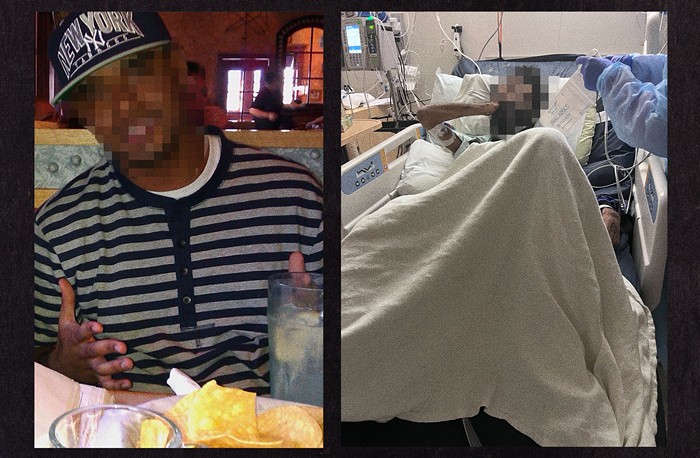
Whatever I thought I meant when I said, "Give it to me straight, doc," I wasn't prepared when the radiologist answered, "I thought we would be talking about saving your breast, but now we're looking at whether we can save your life."
Her pronouncement followed a brief mammogram and ultrasound. They were brief because I only have one breast left to examine. A new tumor had been found in it. The radiologist debated aloud whether my cancer was stage IV—sometimes called "advanced" cancer. There is no cure for it. She said they would need a full-body PET scan to make a diagnosis. The ultrasound had already shown that cancer had migrated into my axillary (underarm) lymph nodes, and in a recent upper-body MRI scan, suspicious spots, probably cancer, were visible on the top of my liver.
I couldn't get my mind around the words she was using: "foreshortened life," "chronic," "stage IV." I needed a filter. I needed music. I often ask doctors if I can use music to help me through situations like these. But where were my earbuds? Were they in my computer bag? And where had I put my phone?
Earlier, waiting in the Swedish Breast Center lobby, I'd watched a woman walk in dazed circles looking for her phone, and the whole office staff and most of us patients joined the search. I'd looked under my chair cushion. Clearly, the woman had received a lousy diagnosis. Her phone was probably sitting at the bottom of her purse, or on her kitchen counter, or on the front seat of her car, ringing and ringing. She'd said she couldn't remember where she'd parked. The mind flips course in shock, circling like a grieving bird around a buoyant emptiness.
The radiologist kept talking, but my capacity to translate information wasn't keeping pace. My partner found the earbuds and the phone with its minimal collection of music. I scrolled to Mary J. Blige's "Sweet Thing," and pressed play. I had it on very low volume, but I had it, and I needed it—needed paradox, something upbeat, a transport, a sweet voice calling up lost love, a steady rhythm to slow my heartbeat. The familiarity of the music calmed me down enough to be able to receive what the radiologist was saying.
Her next step was to shoot tiny metallic markers, which felt like thick staples from a staple gun, into my right breast. The markers remain in tissue to track whether the tumor grows or shrinks with treatment.
I'd had a mastectomy 10 years ago, but the radiologist clarified that the new cancer wasn't the same "barely-stage-I" variety I'd been diagnosed with back then. The two cancers had nothing to do with each other. They were fed by different kinds of hormones, "which—sorry to say," she said, "makes you particularly unlucky." That cancer 10 years ago had been caught early and was easy to contain and excise. This new strain was aggressive, reproducing fast. It was definitely an emergency. This was early December of 2013, and already I was thinking that the coming Christmas might be my last. She scheduled an urgent PET scan to get more detailed images of my liver.
I had the strange sensation of my internal world—synapses, blood rhythms, identity, aspirations—shifting in response to the gravitational pull of a new and precarious orbit. Since the first round of cancer in 2004, I had warned friends and family that if it recurred I would probably refuse traditional treatment. I hadn't quite decided what I would do instead. Go to Germany like Farrah Fawcett for treatments unproven or unreplicated, and thus restricted in the US? Visit a retreat center somewhere in the Himalayas or Marin County to meditate, get daily colonics, and go paleo? I had reached a reactive tipping point somewhere during those 10 years where reading about cancer in magazines or listening to cancer treatment ads on the radio irritated me, like constant nagging.
That cancer diagnosis came at a lousy time: My toddler nephew was dying from brain cancer. My brother and his wife were devastated; they'd tried every available treatment and cure including experimental laser knife surgeries. Their last effort was to dip their 3-year-old son in the legendary healing waters at Lourdes. My situation, in comparison to that, seemed random and vague—I'd had no symptoms before I was diagnosed at my first-ever mammogram with ductal carcinoma in situ, and anyway, I didn't trust the doctors' zeal for swift and preventative measures. I initially resisted their treatment prescriptions (excising tissue and lymph nodes) as a kind of medical colonization of my body. Everything seemed political to me back then. I considered myself an unwitting traveler in what Susan Sontag called the "kingdom of illness" at the beginning of her pivotal 1978 book Illness as Metaphor.
Sontag intended to mock illness metaphors—including that kingdom one. But her highbrow attempt at irony backfired because she conjured up an illness metaphor that resonated. Her literary double-backflip has largely been forgotten, and the powerful kingdom metaphor abides. She was attempting to deconstruct the dangers of metaphors that arise in relation to diseases whose causes are obscure, to purge us of metaphorical thinking and toward a strictly clinical approach, but she wasn't exactly immune to metaphorical thinking herself. This is someone who'd written in Partisan Review in 1967: "The white race is the cancer of human history."
Sontag advocated for the elimination of any symbolic language around diseases that might fuel prejudice or misunderstanding, or obstruct the search for clinical answers. This provided useful intellectual ballast during the AIDS epidemic, which the Reagan White House famously saw as punishment for sexual deviancy. As a postmodern advocate for science and its measurable truths, Sontag preferred precise and sanitized medical explanations over religious, literary, or cultural ones. She bristled at the portrayal of cancer as a battlefield enemy to be conquered through "war."
But she wasn't entirely right. In my view, metaphors may be as essential for humans as are light, shelter, and food. The battle metaphor will remain in the public discourse until we actually DO decode and cure cancer, which, like terrorism, seems to grow cells in secret, change, and evade, and as with the war on terror, the rhetoric brings urgency and a sense of purpose to the work.
Despite Sontag's insistence that there's always a clinical explanation, there isn't, not yet at least: Cancer arrives and disappears mysteriously. Its origins have been traced, among other things, to environmental influences and genetic tendencies. Perhaps cancer is a transient phenomenon in our bodies, which radicalizes once, or where, our immunity is weak. Recovering from and living with cancer is also mysterious; whether we like it or not, it often involves the reconstruction of a self, which involves language.
Illness as Metaphor was fueled by a clarifying rage. Sontag underwent a radical mastectomy, extensive radiation, and 30 grueling months of chemotherapy for stage IV breast cancer between 1974 and 1977. It's no surprise she sought intellectual refuge in a clean medical world wherein humans could rise above primitive aspects of their bodies. In Illness as Metaphor, published in 1978, there is some worthwhile thinking and writing, but it's laced with disdain for anyone who doesn't think like she does. She takes unnecessary potshots, for example, at Wilhelm Reich and Georg Groddeck, both of whom had already been banished to the historical fringes of medicine, and both of whom argued that illness was to some extent self-determined. Sontag rightly named such thinking as morally dangerous because it could easily lead to blaming an ill person for being ill and for failing to recover.
On the other hand, Sontag's quick and total dismissal of Reich and Groddeck was facile. They weren't merely eccentric buffoons, as she'd have you believe. I do not have space in this essay to rectify Reich's tainted reputation, although some of his theories—at least his views on character structure—are well worth revisiting. Groddeck, who inspired Freud's concept of the id, advocated for treating illnesses by addressing the intersections between mind and body, such as when he combined analysis and massage. Groddeck also asserted that the urge to symbolize—the urge toward metaphorical thinking—was essential to human development and healing.
Frankly, Groddeck's ideas about the power of metaphor have been much more appealing and comforting to me over the last year than Sontag's sterile terrain. Yes, metaphors can be used as blunt instruments to shut down discourse and short-circuit critical thinking. But metaphors also have the power to transcend and sometimes transform illness and other lousy human experiences. I think of my brother dipping his dying son in the waters of Lourdes, as he stood with his wife and hundreds of other desperate people dreaming of an ultimate cure. His son died a few weeks later. The waters were the symbolic moment that launched and carried them into grief, and helped them start to make sense of the unfathomable.
I'm not the first person to think this. Much has been written since the 1970s about how mind and body may be intertwined in what makes us sick and what heals us. Recent books like Anticancer: A New Way of Life and Radical Remission assert the importance of such activities as releasing suppressed emotions, accessing social support, eating whole foods, exercising, and meditating as part of what may be both preventative and curative.
As I've been wrangling with Sontag's thinking over the years—she would sneer about releasing suppressed emotions or eating whole foods—I've simultaneously come to doubt whether I ever needed that first mastectomy. I keep returning to empirical counterarguments like Gilbert Welch's New York Times op-ed from November 2012: "Cancer Survivor or Victim of Overdiagnosis?" The Dartmouth-based researcher questioned whether 1.5 million additional women receiving early stage breast cancer diagnoses directly correlated with statistics about more women's lives being saved. Welch speculated that credit was more likely due to the dramatic improvements in the overall treatment of breast cancer since the late 1990s, such as the advent of targeted hormones and antibodies.
All arguments, all evidence, all arrogance about my own opinions built up over the last 10 years dissolved in that pivotal instant when tumors returned, when I was lying on the examining table in the radiologist's office being given a provisional late-stage cancer diagnosis. My first thought—when faced with the possibility of impending death—wasn't: Oh, yeah, I'm going to refuse treatment. My first thought was about a promise to stick around that I'd made to my partner's daughter.
Over the singing of Mary J. Blige, I announced aloud to the radiologist, "I'll do whatever it takes. Chemo. Radiation. Surgery. Losing my hair..." She stopped talking. I was yelling in her ear.
You would think hair is of no consequence, but mine was part of my persona—big, red, and unruly. I liked to hide in the mess of it. I had nearly the same hairstyle for 25 years. The thought of losing it was akin to a loss of self. But losing that was only the beginning.
The first guiding metaphor that helped give order to what was coming was something one of my doctors said. He compared being diagnosed with stage IV cancer to stepping onto a roller coaster car in a dark enclosed space. Once the diagnostic bar comes down and the car starts rolling, there's no time to think. There's just shock at the prospect of death.
My first serious medical appointments happened over Christmas. The holiday was a lush island in a lake of fog. I found myself craving Christmas carols, staring fondly at the neighbors' ostentatious display of lights, and listening to the rhythm of conversations, enjoying that—just voices—without caring what anyone said. I had some catastrophic thoughts and some morbid thoughts, and drank a few glasses of wine—a brief and final indulgence.
The day after those glasses of wine, I looked at my liver. Well, first I watched my oncologist look at my liver, on digital scans. He resembled Kurt Vonnegut with tousled silver hair and glasses above his brow. I liked him immediately, which was unusual for me. Ten years ago, I had walked out on an oncologist who was matter-of-fact, technically proficient, and told me, disdainfully, "Naturopathy is quackery." This new oncologist had a more human approach. He sat with his chin in his hand looking forlornly at my beleaguered liver.
"I don't like these much," he said, turning the computer screen towards me. "Want me to show you what's going on here?"
He might as well have said, "Here is the image of your unconscious." Visceral organs, whether or not they're covered with constellations of tumors, are repulsive and fascinating. Livers and spleens are sequestered away and follow their own strange pulses and functions, as primitive as ancient fish.
The oncologist pointed to various places on the screen to indicate where 50 to 60 tumors had spread across my liver and throughout my abdominal cavity. None were in my brain or bones. My partner took notes on her laptop and asked pointed questions. I sat staring blankly at the screen. Fifty to sixty tumors? How's that possible? The oncologist sat with us for two generous hours telling cancer victory stories. The girl who got pink wigs from a stripper supply store. The women who were living great lives in remission.
My medical records were all stamped "Urgent" in red ink. The oncologist said, "You need to start right away." I was hoping "right away" meant two to three weeks—I had to tell my family and warn my employer—but it didn't, it meant four days. Really, I just wanted the roller coaster to slow the fuck down for a second, but it was already under way. I had the distinct feeling of someone of some notable weight—God; or the winged, sword-wielding archangel Michael; or the older, denser Marlon Brando—standing squarely on my chest. I was pinned to a place, to an hour, to a long, drawn-out breath.
I started chemotherapy on New Year's Eve. It wasn't the worst holiday I've ever had. (The worst holiday I've ever had was when I was 21 years old, on a ship from Dublin to Le Havre, en route to Paris, where I would work as a nanny for a snotty rich family. I was sick as a dog, and lonely, and lost at sea within, lost in a psychological wound that I'm not going to talk about but that made letting anyone close impossible.)
Fast-forward several decades: It's New Year's Eve 2013 in the oncology unit at Swedish Hospital. There was the obvious drag of spending the eve of a brand-new year hooked up to a machine pumping toxic chemicals into my bloodstream for eight hours. Despite that, the holiday was memorable, by which I mean full of meaningful human connections. It began with a surgical procedure. The pre-surgery nurse had impeccable comic timing. The surgeon patiently explained the strange portacath tendrils she would thread through veins above my heart. The chemo nurse stayed for a second shift because the hospital was short-staffed. My partner brought Thai food. It was the first night I realized the importance of welcoming help to the point of letting it take off its boots and put its feet up.
That was the beginning of six and a half months of weekly chemo doses. The treatments felt as if essential electrolytes like sodium and potassium were being leached out of my cells and replaced with a repulsive antifungal formula—or something equally toxic—that cleansed while compromising the integrity of whatever it touched.
I won't pretend I was a warrior. I worried. I woke at night and wondered what was going on inside my body, whether I would survive the year. I listened to Beethoven during chemo treatments. A friend had given me a Fidelio CD and a paper he'd written about the opera. I occupied my mind working on a book about using music to build rapport with psychiatric patients, especially with people experiencing psychosis. I was learning that listening to music was sometimes more effective than communicating through speech. Music is its own emotional language that can make order out of chaos, intimacy out of isolation, and meaning from fragments.
Beethoven was the right size and intensity for the mixture of feelings—betrayal, shock, grief, fear, anger, ambivalence, and longing—that late-stage cancer inspired. Fidelio conveyed the pain of suffering and loss, and the transcendence of suffering for the sake of a higher order. It even helped to have the allegorical image of Beethoven's beloved French Revolution—the music's crashing, thematic conflicts—to make sense of how chemotherapy agents, Taxotere and carboplatin, were destroying rogue cancer cells and healthy cells at the same time, and antibodies like Herceptin blocked new cancer growth. Beneath all of it was this emergent sense of another life force arising in me, an interior self (like a new French democracy) distilling down to a thin line. A leitmotif. A violin string thrumming through turbulence.
In some ways, chemotherapy—and its circus of side effects—was easier to contend with than accepting endless gestures of human kindness. A homemade chocolate cake carried through the snow. A partner who navigated through medical bureaucracies with the same fierce grace she used to trail run 50 miles on her 50th birthday. There was meal after meal left in a cooler on my porch at home. An East Coast journalist friend researched cutting-edge medications and then convinced my insurance company to pay for them. There were knitted hats and scarves and balms and concoctions for when my hands and face turned lobster-like and my fingernails fell out. My partner's daughter made me laugh through imitation: wearing my knitted hats, giving me nicknames like Cancer Barbie or Chemo Princess. Her bluntness brought ordinary reality back into the house, just like that homemade cake did, even though I couldn't eat it. No sugar.
Throughout chemotherapy treatment, I kept going to work. As a psychologist who manages a psychiatric outpatient program, I facilitate groups of people struggling with a variety of mental health concerns, including suicidal urges. I was desperate to live, unlike many of them, but it would be too simple to say we were coming from opposite directions. In truth, we shared common risks.
Of course, a cancer diagnosis is quite different than a major mental health diagnosis. Depression and PTSD can't be measured on CT scans. Having a mental illness is even more intangible and mysterious than having cancer. And it is easier, far easier, to "come out" with stage IV cancer than it is with schizophrenia or bipolar disorder. It's also easier to get treatment. The recently released Mental Health America report Parity or Disparity: The State of Mental Health in America 2015 shows that Washington State is rated 48 out of 51 states (the report includes the District of Columbia) in terms of people's access to mental health care in relation to need. Mental health issues can worsen the prognosis of a range of other physical illnesses like heart disease, diabetes, and cancer. Isolation and lack of mental health care can lead to fatal ends. A recent study from the University of Oxford found that serious mental illness reduces life expectancy by 10 to 20 years.
Unlike with mental illness, people rally in tangible ways around someone with a cancer diagnosis. They bring food. They walk the dog. They sit with you through the dull drip hours of chemotherapy. A diagnosis of major depressive disorder, bipolar disorder, or psychosis does not usually inspire casseroles. There's no plethora of family-friendly diet guides for lithium takers, no relaxation audio books for voice-hearers, no lavender eye pillows for people experiencing visual hallucinations. But there are so many cancer support resources targeted to various demographics that I can find 17 different ways to save my cuticles, or freeze my hair so it won't fall out. If we can agree that facing our mortality is terrifying, consider losing control over your own mind.
Another irony of facilitating therapy groups, as I do each day, was that I actively needed to practice the coping tricks I was teaching. Those coping tricks include listening to music, breathing, meditation, affirmations, and paying attention on purpose (aka mindfulness). Suddenly, none of this was theoretical or abstract. Sometimes—especially at 5:30 a.m. on a Monday morning after a weekend of chemo recovery—my coping techniques fell apart, or they didn't work fast enough. So I did what I had always advised patients to do, which was do them anyway. Or try something else. Or try two techniques in combination. I threw the book of daily aphorisms written by a former elementary school teacher who became a Buddhist nun across the room, as I'd encouraged my own patients to throw it if it irritated them. Later, I picked it up and opened to a different page.
And I faced squarely the ways I had been holding myself back from life and from self-expression. At my job, I would often ask patients to consider reconstructing stories they told about themselves. I began to understand that illness or compromised health has its own reconstructive process. Illness unmakes us and remakes us regardless of our best-laid plans. I had the choice of assenting or resisting. Accepting help has made it easier to let go of things I once fiercely defended: my righteous indignation, my precious fears, my pride, my hair.
I circled around barber shops for weeks before I finally walked into an anonymous one on University Avenue. I took off my blue knit hat. The stylist asked if I'd thought about shaving my head for a long time. She didn't notice the bald patches. She didn't assume I had cancer. It was a relief: the stylist's indifference, the locks of hair falling to the floor. It turned out that my head was a pretty decent shape. No bumps. I put the hat back on, paid her, and walked away. I didn't have any emotion until I got back behind the wheel of my car. Then I felt incredibly sad; I drove around the block several times, listening to Bob Dylan, not knowing where to go next.
"You really looked like shit last week," one of my coworkers said on a Monday morning, three months after chemo started. People tended not to tell me when my eyes were sunken or my face was blotchy red or my nose dripped blood on the mahogany boardroom table. Nor did I try to hide behind wigs or makeup.
Instead of avoiding the topic of cancer like I had done the first time around, I immersed myself in the culture. I read Audre Lorde's journal, Virginia Woolf's treatise on illness, postcolonial meta-analyses of illness narratives, websites, and magazines. I looked at chat groups and blogs and cancer websites. I quit fighting the word "survivor," which had always seemed to me to tempt fate. I corresponded with women who had been through similar stage IV experiences. I gratefully accepted prayer shawls, bag balm, and green totem stones. Who knows what cures us?
I started listening to Max Richter's version of Vivaldi's Four Seasons over and over, trying to discern the patterns. I dipped back into Beethoven when rougher emotional waters roiled, but the rearrangement of Vivaldi's classic seemed closer to an interior reinvention, like the softer insistence of water reshaping a stone. I also found comfort in an essay by the musician and psychoanalyst Emanuel Ghent, who referred to the necessity of "surrender" in the process of regaining health. Ghent meant assenting to the truth of a difficult matter at hand. The transcendence in Ghent's version of surrender included arriving at a broader perspective within which a person could also experience being embraced. I suppose that sense of being held could be God, if you leaned that way, or Nature. It could also be an awkward, sweaty hug from Marlon Brando. (I don't why that actor's image keeps coming to mind—another mystery.)
For me the sense of being contained by something bigger than myself came from leaning into Keats and Beethoven—artists who strove, despite pain, to hold on to aesthetic ideals. Keats advocated for letting meanings unfold instead of grasping after facts or desires. Today, we would probably call this pursuit "mindfulness." Keats called it "negative capability." He wrote a letter about it to his brother, who was dying of tuberculosis—the same disease that ultimately claimed Keats's life. Negative capability was the invention of a man who intimately understood being abandoned by desire and passion, but inviolately believed in them anyway.
There was a threshold day during chemo where all food and beverages, even water, began tasting like metal and cold potatoes. At that point there didn't seem to be a future, only an endless repetition of rogue cells infiltrating tissues and organs, along with the steady fading away of passion. That was a dark and a clarifying place, a distillation that evolved into a feeling that approached purity. My body was broken down to the point that it needed to restart again. I was hairless. I didn't sweat. Even the idea of sex seemed exhausting. All of my adamant beliefs crumbled.
I became more keenly aware of how many people were wrangling with serious health issues, and how isolating illness can be when you are living in it. The urge to belong and make meanings abides in us. Metaphors are great connectivity devices that viscerally convey, even if we don't yet comprehend, big emotional experiences. Illness awakens symbols in us by which we make sense of ourselves, and our experiences. The closest I can get to an explanation of what I mean here is by describing the culminating crisis of my stage IV cancer.
It happened in late April, four months after the radiologist suggested that my life needed saving. It was my second scheduled scan; the first one had shown slow, steady reduction in tumors—nothing dramatic. This second CT scan showed that something odd was growing in my lungs. A CT scan shows where there are densities in tissue, and densities can indicate tumors or other growths, but CT scans don't show whether such growths are cancer. Neither my oncologist nor the radiologist could discern whether the invading agent was a new cancer, an infection, or an allergic reaction. I got a second opinion that week from an oncologist who said "new tumor" so many times it felt like something had actually grown—something fear-conjured to the size of a cantaloupe—in my lungs. She was pretty certain cancer had metastasized to my lungs, and this was the evidence of it; she also predicted that my liver was in much lousier shape than it had been in December, when those 50 to 60 tumors were spotted.
In the meantime, Dr. Vonnegut scheduled a more informative test, a PET scan, which involved fasting and then drinking a sugary drink and then getting a dose of radiation: This would end up creating three-dimensional color images of body functions and processes. Basically, sugars are drawn to active tumors and lesions. The doctor was hoping for clarity about what was going on in my lungs. Unexpectedly, the PET scan revealed that there was no active cancer in formerly disease-ridden sites, that even my liver looked good, but that whatever was growing in my lungs had doubled in size.
In order to figure out the lung mystery, I was admitted to the hospital for a series of tests, including a needle biopsy of my lungs. This procedure involves having a needle inserted in a lung to extract a tissue sample, and the main risk of it is that the lung might get punctured and collapse. Various medical professionals estimated the risk of a puncture was anywhere from 1 percent to 30 percent. All of them agreed that the pain from a punctured lung was "excruciating." I took all precautions, including accepting the hospital chaplain's offer to pray over me. He held my hand. It was awkward.
The day of that lung biopsy played out like a rock opera of linked metaphors. First, it felt like a MASH episode. It was a bustling afternoon at the surgery center. I waited an eternal hour on a rolling transport bed. Then a tidy, bespectacled surgeon gave me a pep talk about the CT-scan-guided needle-biopsy procedure. He assured me collapsed lungs were rare. He asked me to sign an authorization. I got his permission to listen to my iPod during surgery.
I was wheeled into a sterile white room and transferred to a platform bed that could slide into an MRI machine. Wait. What? "The surgeon said a CT scan, didn't he?" I asked. Sure enough, I was in the wrong room, about to be put into the wrong machine. I was unbuckled. The warm blankets came off and I was rolled back to the waiting room. I was grateful to have not lost a body part in that transaction.
Next, a butch, wizened nurse grabbed my gurney bed and yelled out, "Let's rock and roll." We careened down the hallway. "Let's rock and roll" is one of those classic lines that shows up right before troops deploy, or before a mafia massacre. I was having second thoughts. I wished I'd requested a Buddhist monk or watched The Godfather as preparation.
The sedating nurse said I'd soon start to feel the calming effect of sedatives. In the meantime, she and her cohort tried to squeeze my contorted body through a narrow CT scanner, which would snap digital images of my lungs to help guide the surgeon's sampling needle. He needed to extract a small sample of tissue from one of the inflamed areas in my lung. My shoulders scraped the sides of the scanner. "Raise your arms. We're going to put bracelets on you," another nurse said. "Bracelets" was a euphemism to describe Velcro straps that bound my arms above my head. It was an uncomfortable posture; the sedatives hadn't kicked in.
Then the surgeon reappeared. I noticed he had some kind of dried gunk on his glasses. It looked like interstitial fluid mixed with blood. Through the vague gauze of insufficient sedatives, I felt a rising dread. The surgeon sat down behind me. He explained that he would numb my back at the place where he planned to insert the needle. It would be simple. Right before the needle went into my lung, an image of the French artist Odilon Redon's painting of St. Sebastian flashed across my mind, unbidden. The painting depicts the patron saint of gays and the afflicted with his arms tied by rope to a tree branch high above his head. The background is smoky blue. There's a wound in his side. I thought, "That's weird. Maybe this is a bad day for this thing."
At the same time, the surgeon said something indecipherable and a dull, intrusive object—a straw, I later learned—was shoved between my ribs. Apparently the surgeon had just punctured my lung. That would explain the pain. My lung collapsed. The straw was inserted to drain the lung cavity so that the lung could gradually reinflate again. That process would take a few days. It was so painful I found it hard to breathe.
The rollicking nurses rolled me back to the waiting room, where they left me. Oddly, in spite of the intense pain, I wasn't angry. In retrospect, I think the linked associations of the experience—the MASH episode, the painting of St. Sebastian, and Nick Drake, whom I'd been listening to all the while—were doing a better job than the minimal sedatives to make the pain tolerable.
When I returned to my room upstairs, there was more commotion. The lung drain had been set up wrong. I wasn't getting much air. The nurses couldn't give me pain meds until the air problem was fixed. I had the strange sensation then and later that the collapsed lung was... I don't know... a kind of cathartic experience. I know that is counterintuitive.
I'm wondering if it works like this: A formerly ineffable experience—one involving anticipation of pain and a sense of no control, an impression buried deep in implicit memory—had finally found a present-tense experience wherein it could be expressed. One corner of an old broken thing inside was under repair through being recycled, witnessed, and tended. Some part of healing is private and indirect. This is true in mental health as well.
All pain disappeared two days later when the straw was pulled out. Fortunately, the surgeon had extracted enough tissue to send to a lab. It was hard not to jump to worst-case scenarios, but I tried to control myself. The oncology pulmonologist didn't have results yet when I got to his office the following Monday afternoon. He stepped out to call the pathologist, then returned with the news. The stuff growing in my lungs—"organizing pneumonia," he called it—was an allergic reaction to a chemotherapy agent. It was definitive: There was no cancer in my lungs. I dropped my water bottle on the floor and cried.
If the scans and tests were all true, that meant I was in remission.
My tears of relief lasted until the doctor explained the treatment for organizing pneumonia. It required a high dose of steroids for six weeks, then an additional six to seven weeks to taper off them. I said, "No way, I hate steroids!" My partner gave me one of those "You're kidding... right?" looks. I'm not quite sure why I balked at steroids after having endured gallons of toxic chemicals for six months. It was one more chance for choice, one last grasp for control before letting go. I started prednisone a few days later.
What I call remission, my oncologist calls "no evidence of disease." We're both talking about a reprieve. There's no guarantee that cancer won't return. In fact, once cancer metastasizes through lymph nodes to other organs, it's more likely to follow a similar pattern again. Fifteen years ago (before antibodies like Herceptin existed), I would have been dead by now. Fifteen years from now, chemotherapy may be archaic. Vaccines and even more precisely targeted antibodies are plausible. In the future, there will also be other, better words for chronic states of being not exactly ill, but not exactly well.
Recently, I spoke to a friend who has lived with an HIV/AIDS diagnosis and a compromised immune system since the early 1980s. Just like me, he had initially not anticipated surviving. For years he had lived a suspended life, waiting for death, which he regrets now because he foreclosed on things like romance. He described his heightened vigilance about tracking changes and anomalies in his body. I could relate to that. One day I'm grateful that my eyelashes are growing back. The next day, the bruise on my hand is taking way too long to heal. Maybe it's not a bruise at all.
My partner and I drove by the Oso mudslide site a few months ago on our way home from Eastern Washington. The hill that collapsed, burying an intimate community and 41 souls, was smaller than I had expected. The quiet was so thick. Where the sky met the road there was a brand-new barrier to keep a mind from drifting into the emptiness anguish opens. At the nearby store where we stopped for coffee and gas, a man sat under a tribute poster to people who had died or who had joined the rescue efforts. The man told about the fateful day in March and the friends he'd lost. He was drunk. I imagined him repeating the same story to everyone, suspended as he was in eternal shock and haunted by the randomness of survival.
I'm considering a clinical trial with a new cancer vaccine. I am interested in keeping current on cutting-edge treatments and other clinical solutions to cancer. I go to the Arnold Pavilion at Swedish every three weeks for doses of antibodies. But I don't rely completely on empirical science as my savior. I get acupuncture and visit an analyst who reminds me that "it could happen to any of us" when I'm sidelined by fear of recurrence. He's right, of course. We don't really enter the kingdom of illness; it enters us, and we can't always know from where and what form it takes.
Whenever I start to feel trapped, I dial the iPod to music that makes sense of things. Lately, it's been John Prine singing, "Make me an angel that flies from Montgomery/Make me a poster of an old rodeo/Just give me one thing that I can hold on to..." ![]()