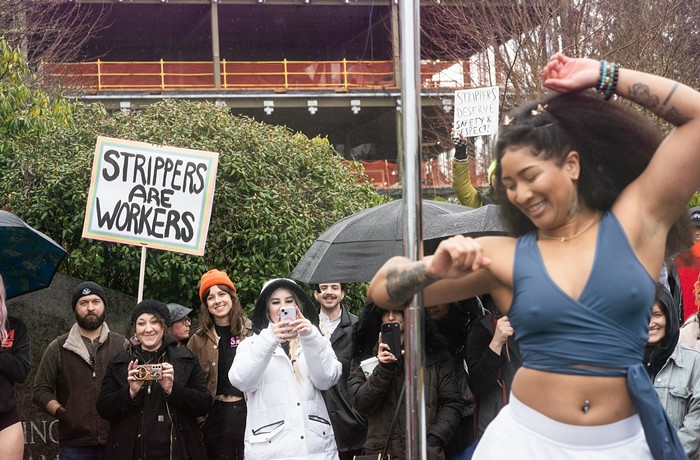Washington State Insurance Commissioner Mike Kreidler sent a landmark letter to all health-insurance carriers in the state today that bans the longstanding practice of denying coverage to transgender people for the same treatments available to nontrans policy holders. Not only are are such heath care exclusions now considered "prohibited" under state law—in cases where cisgender people would be eligible for the same services, such as surgeries and hormone treatments—Kreidler says people wrongly denied coverage will be encouraged to report their health care provider for investigation.
The Coalition for Inclusive Healthcare, a large constellation of pro-trans organizations that has been working behind the scenes for these reforms, praised the decisions as necessary because "private health insurance policies routinely include clauses that specifically preclude transgender people from accessing medical and mental health care that is covered for other policy holders."
"Nearly all insurance plans in Washington categorically exclude coverage for transition-related medical treatment, even when that same treatment (such as mental health care or hormone replacement therapy) is covered for non-transgender people," the group says in a statement. Also be sure to read the
CIH's FAQ on the decision.
Kreidler's letter, which explains his office's reasoning, appears in full after the jump. In short: A combination of state anti-discrimination law and federal health-care law now make denying equal health care legally indefensible. "Reading the provisions of state law in conjunction with the definitions contained in Washington state’s Law Against Discrimination, and the requirements of the federal Affordable Care Act," Kreidler writes, "it is clear that exclusions, prohibitions, and other forms of discrimination by issuers against policy holders who identify as transgender is prohibited."
Awesome. Awesome. Awesome.
MIKE KREIDLER
STATE INSURANCE COMMISSIONER
June 25, 2014
OLYMPIA OFFICE: INSURANCE BUILDING P.O. BOX 40255 OLYMPIA, WA 98504-0255 Phone: (360) 725-7000
To Health Insurance Carriers in Washington State:
STATE OF WASHINGTON
OFFICE OF INSURANCE COMMISSIONERThe purpose of this letter is to clarify prohibitions in Washington State against discrimination in insurance coverage on the basis of gender identity or gender dysphoria.(1)
Recent changes in policy at the federal and the state level relating to transgender health care services, coupled with the potential harm to consumers arising from the denial or exclusion of services on the basis of gender identity and related medical conditions, has prompted a review of transgender health care service exclusions and denials in plans licensed or regulated by the Insurance Commissioner’s Office.
As described in further detail below, broad exclusions of coverage on the basis of gender identity are prohibited under Washington state law. Additionally, denial of a medically necessary service on the basis of gender identity is prohibited under Washington state law.Section 1557 of the federal Patient Protection and Affordable Care Act (ACA)(2) provides that an individual shall not be “excluded from participation in, be denied the benefits of, or be subjected to discrimination under, any health program or activity, any part of which is receiving Federal financial assistance, including credits, subsidies, or contracts of insurance, or under any program or activity that is administered by an Executive Agency or any entity established under [Title I of the Patient Protection and Affordable Care Act.]” on any of the grounds prohibited under various federal discrimination provisions.
The Department of Health and Human Services Office of Civil Rights (OCR) is responsible for some enforcement of Section 1557 of the ACA. In a July 12, 2012 letter (3) to the National Center for Lesbian Rights, OCR clarified that sex-based discrimination includes discrimination on the basis of gender identity and sex stereotypes under Section 1557 of the ACA. OCR agreed that Section 1557’s sex discrimination prohibition extended to claims of discrimination based on gender identity or failure to conform to stereotypical notions of masculinity and femininity. The section also prohibits discrimination regardless of actual or perceived sexual orientation or gender identity of the individuals involved.
At the state level, Washington state’s Law Against Discrimination, codified at Chapter 49.60 RCW, prohibits discrimination based upon sexual orientation, which includes “gender expression or identity,” defined as “having or being perceived to have a gender identity, self-image, appearance, behavior, or expression, whether or not that gender identity, self-image, appearance, behavior, or expression is different from that traditionally associated with the sex assigned to that person at birth.” RCW 49.60.040(26).
Washington state law expressly prohibits discrimination based on the “sex, marital status, or sexual orientation as defined in RCW 49.60.040, or the presence of any sensory, mental, or physical handicap of the insured or prospective insured.” RCW 48.30.300. This prohibition applies in the issuance, cancellation, or renewal of any contract of insurance, as well as amount of benefits payable, or any term, rate, condition, or type of coverage offered. RCW 48.30.300. While discrimination based on certain classifications is permissible “when bona fide statistical differences in risk or exposure have been substantiated,” sexual orientation, including gender identity, is not one of those permitted classifications of discrimination.
The prohibition in state law against discrimination applies “notwithstanding any provision contained in Title 48 RCW to the contrary.” RCW 48.30.300. This phrase indicates that the nondiscrimination requirement applies throughout state law. As such, provisions of Title 48 RCW that could otherwise be seen as permitting broad exclusions of health care services related to gender identity should not be used for this purpose.Reading the provisions of state law in conjunction with the definitions contained in Washington state’s Law Against Discrimination, and the requirements of the federal Affordable Care Act, it is clear that exclusions, prohibitions, and other forms of discrimination by issuers against policy holders who identify as transgender is prohibited.
The Insurance Commissioner’s Office will review filings and coverage for prohibited exclusions and for whether medically necessary services for transgender individuals are covered to the same extent that those services are covered for non-transgender individuals enrolled in the same plan. Additionally, those affected by exclusions and denials of service will be encouraged to contact the agency so that specific issues can be investigated and addressed.
This letter serves as a reminder that Washington state law affords policyholders who identify as transgender the full measure of benefits under health insurance policies as individuals seeking medically necessary treatment for non-gender identity related conditions.
Questions about this letter should be directed to Jason Siems, Deputy Commissioner for Policy and Legislative Affairs, jasons@oic.wa.gov or (360) 725-7037.
Sincerely,
Mike Kreidler Insurance Commissioner1 Gender dysphoria (formerly known as gender identity disorder) is a condition based on the gender identity or expression of the insured. See, e.g., Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition, Code 302.85 (gender dysphoria is a “marked incongruence between one’s experienced/expressed gender and assigned gender, of at least 6 months’ duration,” as manifested by certain criterion).
2 42 U.S.C.§18116.
3 HHS Office of Civil Rights letter dated July 12, 2012.